The names of the knee ligaments
The principle ligaments of the knee are as follows:
Knee Ligaments Animation
Anterior cruciate ligament - ACL
The anterior cruciate ligament is a made up of two bands of fibres lying centrally within the knee joint passing from the front (anterior) to the back (posterior) of the knee. It is attached at its lower end to a little depression in the central part of the upper tibia. This is its anterior attachment. From there it leads upwards and backwards to the inner part of the lateral femoral condyle which forms its posterior attachment. The two bands of fibres are aligned so that one band becomes tight in rather more flexion and the other band becomes tight in more extended positions of the knee. The ACL contributes to control of knee movement so that the joint surfaces of the tibia remain properly aligned to the femur in all stages of knee bend. Without it the tibia becomes unstable in relation to the femur and tends to slide forwards under load disturbing the normal pivoting action of the knee joint. The ACL also contributes to rotational stability of the knee.
ACL Animation
Posterior cruciate ligament - PCL
The posterior cruciate ligament is considerably thicker and stronger than the ACL and is also made up of two bundles of fibres. These pass forwards from the back (posterior) to the front (anterior) of the knee. It is attached at its lower end to quite a broad area of the back of the upper tibia. This is its posterior attachment. From there it leads upwards and forwards ending up attached to the inner part of the medial femoral condyle which forms its anterior attachment. The two bundles of fibres are also aligned so that one band becomes tight in rather more flexion and the other band becomes tight in more extended positions of the knee. Like the ACL the PCL contributes to stabilisation of knee movements so that the joint surfaces of the tibia remain properly aligned to the femur in all stages of knee bend. Without it the tibia becomes unstable in relation to the femur and tends to slide backwards under load.
PCL Animation
Medial collateral ligament - MCL
The medial collateral ligament is on the inner (medial) side of the knee. It is quite a wide ligament that passes from the medial aspect of the upper tibia at a point 4 to 5 cm below the knee. From there it passes upwards to join the medial femoral condyle quite far around the side of the condyle. It also has two bands. The superficial layer which is heavier and broader and a deep layer which is much thinner and which attached to the medial meniscus. The MCL controls sideways movements of the knee and without it the knee tends to give way on the inner side that is the knee goes into a valgus (knock knee) alignment under certain types of loading.
MCL Animation
Lateral collateral ligament - LCL
The lateral collateral ligament is on outer (lateral) side of the knee and is sometimes called the fibular collateral ligament. It is more rounded and slimmer than the MCL and stands away from the joint unlike the MCL which runs quite close to the underlying bone. It is attached at its lower end to the head of the fibula and at its upper end to the lateral femoral condyle slightly towards the back of the condyle. The LCL controls sideways movements of the knee and without it the knee tends to give way on the lateral side, that is, the knee goes into a varus (bow leg) alignment under certain types of loading. It also contributes to the posterolateral corner (see below).
LCL Animation
Postero-lateral corner - PLC
The structures of the posterolateral corner jointly act as a check ligament to control movement of the lateral side of the knee joint. Another name for these structures is the posterolateral complex reflecting the fact that there are a number of structures that contribute to it. The three main structures involved are the LCL, the popliteus tendon, and the popliteofibular ligament. The bony shape of the lateral side of the knee makes it inherently more unstable than the medial side and additional stability is provided by the PLC to control sideways movement, and a combination of external rotation and backwards movement of the outer side of the upper tibia. Without the PLC, the knee tends to be rotationally unstable, that is there is an excessive twisting movement of the tibia under certain types of loading.
Degree of severity of ligament injuies
There are varying degrees of severity of ligament injury ranging from a minor sprain or stretching of the ligament through to a complete rupture. The extent of the tissue damage is roughly correlated with the degree of pain, swelling and disability that results and the length of time taken for recovery. With a minor sprain there will be mild to moderate pain and swelling but you will be able to continue walking but may not be able to do anything more strenuous without difficulty. With a partial ligament rupture there will be more significant swelling and often visible bruising. You might still be able to walk but are likely to be in quite a lot of pain and walking distance may well be limited. In most cases of complete rupture of a ligament there is substantial pain and disability and you are likely to require a stick or crutches to be able to walk. The joint is likely to feel unstable and other support may be required such as a brace. Other injuries, such as a meniscus tear, or damage to the articular cartilage are common after complete or partial rupture of a knee ligament.
MCL Injuries
Medial collateral ligament injuries (MCL) are the commonest ligament injuries around the knee. They are sustained in almost all types of sports and affect people of any age. They tend to affect male athletes more so than females and are most common in contact sports such as football, rugby and in martial arts including wrestling and judo. Many MCL ligament injuries are minor sprains that need no treatment.
Examination of a patient with an MCL injury generally reveals tenderness along the line of the ligament and pain on stressing the knee into a valgus (knock knee) position. The integrity of the MCL is also evaluated when stressing the knee into valgus. If abnormal laxity is detected it is compared with the opposite knee as there is some individual variation in the natural degree of ligament laxity. In Grade 1 injuries most of the fibres of the ligament remain structurally intact and there is less than 5mm of medial opening on valgus testing. In Grade 2 injuries there is between 5 and 10 mm of medial opening which implies an incomplete tear. Grade 3 injuries have more than 10mm of opening and this implies a complete rupture. In rare cases the torn end of the ligament retracts and actually gets caught within the knee joint.
Most MCL injuries are treated conservatively but rarely, persistent laxity of the MCL requires surgical repair or reconstruction of the ligament.
ACL Injuries
Damage to the ACL is the commonest cause of instability of the knee. While minor sprains occur quite frequently, a significant number of ACL injuries result in complete or partial rupture of the ligament resulting in quite a high frequency of debility. The ACL can be overstretched either as a result of a contact injury such as a football tackle, but more often as a result of a non-contact injury. Hyperextension of the knee more than10 degrees beyond its normal range or forced rotation as occurs in alpine skiing can both rupture the ACL. Women are more prone to ACL injuries than men. The patient often experiences sudden severe pain accompanied by a popping sound as the ligament ruptures. The knee usually swells rapidly due to bleeding from the ACL directly into the knee joint.
|

|
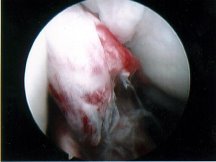
|
|
Normal ACL
|
Ruptured ACL
|
Examining the ACL
Examination of a patient with an ACL injury involves a number of tests. The anterior drawer test is done with the hip at 45 degrees and the knee at 90 degrees. The hamstrings should be relaxed. The tibia is pulled forwards. An increased forward movement of the tibia or the lack of a firm end point is indicative of ACL damage. The Lachman test is done with the knee at 30 degrees of flexion with the examiner steadying the thigh with one hand and using the other hand to draw the tibia forwards. It is a more reliable indicator of ACL laxity than the anterior drawer test. In the Pivot Shift Tests the knee is extended and internally rotated while the doctor applies a valgus force to the knee. The knee is then flexed. A sudden shift in the pivot point occurs as the tibia suddenly shifts backwards to its correct alignment from an anteriorly displaced position. An MRI scan is now considered essential in the evaluation of ACL injury, not only to confirm the extent of damage to the ACL but also to look for associated damage to the MCL, menisci, articular cartilage and associated fractures or bone bruising.
As a rule of thumb about a third of patients can be rehabilitated conservatively following ACL injuries by means of Physiotherapy to build up hamstring muscle power, use of a knee brace during activities such as skiing, and exchanging sporting activities for ‘straight-line’ exercises such as cycling. About a third of patients will have such severe instability that they have frequent giving way of the knee during ordinary daily activities and cannot be rehabilitated without surgery. A further third can manage daily activities without difficulty but find the knee gives way during exercise or sport.
Deciding on the degree of laxity, the age of the patient and their sporting aspirations ACL injuries may be treated conservatively but a significant number require surgical ACL reconstruction which is carried out largely arthroscopically (key-hole surgery). The main indication for surgery is recurrent giving way of the knee. The most popular technique for repairing the ACL involves taking part of your natural hamstring tendons and inserting that as a substitute for the ACL. A number of other possible tissues can be used including part of the patellar tendon. In some cases an allograft is used from a tissue donor. Finally, synthetic ligament substitutes are also available. The choice of material depends on the surgeon, patient choice and the precise circumstances.
ACL Laxity
Isolated PCL Injuries
Isolated posterior cruciate ligament injuries usually respond well to Physiotherapy. If the quadriceps muscles are sufficiently strengthened and maintained through regular exercise this is all that may be needed. However if there is sufficient disability surgical repair may be indicated. The decision to undergo surgery is often a personal choice and the age of the patient, sporting aspirations and physical condition are all considered when making the recommendation for type of treatment. The surgical procedure involves reconstructing the PCL by inserting a tendon graft, either by using your natural hamstring tendons or an allograft which is taken from a tissue donor.
Multi-ligament Injuries including the PLC
Many posterior cruciate ligament and postero-lateral corner (PLC) tears occur in association with other ligament injuries around the year, most notably ACL tears. When this occurs it often leads to quite major instability which requires surgical intervention.
Fortunately these complex multi-ligament injuries are relatively uncommon. When they do occur they are quite difficult to reconstruct surgically and surgery is best performed by a surgeon with a special interest in this type of ligament surgery.
TEXT Copyright London Knee Clinic® 2014